
The Indian motor insurance coverage market is presently valued at round $13.19 billion and is projected to achieve $21.48 billion by 2030. Whereas the business continues to develop steadily, regulators have additionally issued sturdy mandates to insurers to enhance their turnaround occasions and supply higher buyer experiences.
For one in all India’s greatest non-public insurers, which prided itself on a excessive declare settlement ratio, this meant discovering new methods to streamline its back-office processes and scale back guide errors. But it surely wasn’t simple. They course of greater than 350,000 circumstances yearly— every file accommodates over 10 forms of paperwork, various codecs and buildings, 30+ line objects, and a number of ingestion channels. They’d a backend crew of 40 information entry clerks and vehicle specialists manually inputting data from restore estimates, invoices, and supporting paperwork into their declare administration system
This inefficient, unscalable workflow could not meet the regulator’s turnaround time mandates, forcing a re-evaluation of their motor declare processing strategy. Let’s discover how they went about it.
What modified in motor declare processing in 2024
In June 2024, IRDAI, the Indian insurance coverage regulator, issued new pointers aimed toward enhancing motor insurance coverage declare settlement processes.
The important thing modifications included:
- No arbitrary rejection of motor insurance coverage claims resulting from lack of paperwork — insurers should request all required paperwork upfront throughout coverage issuance
- Insurers should allocate a surveyor inside 24 hours, acquire the survey report inside 15 days, and determine on the declare inside 7 days of receiving the survey report
- Necessary buyer data sheet (CIS) to offer clear coverage particulars and claims course of
- Restrictions on coverage cancellation, permitting it solely in circumstances of confirmed fraud with 7-day discover
- Requirement to reveal the insured declared worth (IDV) calculation technique
Because the insurer’s enterprise grew quickly, these regulatory challenges made dealing with near 30,000 claims month-to-month turned greater than only a processing problem. It uncovered elementary operational constraints that threatened their capacity to scale and ship worth to prospects.
Let’s discover how these modifications affected the insurer’s enterprise:
- Couldn’t scale their operations with out including head depend.
- Unable to fulfill IRDAI’s necessary declare settlement timelines – risking regulatory penalties for violations
- Getting poor evaluations and adverse suggestions from prospects
- Car specialists spending useful time on information entry as an alternative of value evaluation
These challenges made it unimaginable for them to justify premium will increase based mostly on precise declare prices and threat profiles.
Why guide declare processing was sophisticated
Let’s first try to perceive what the insurer’s declare processing workflow used to appear to be.
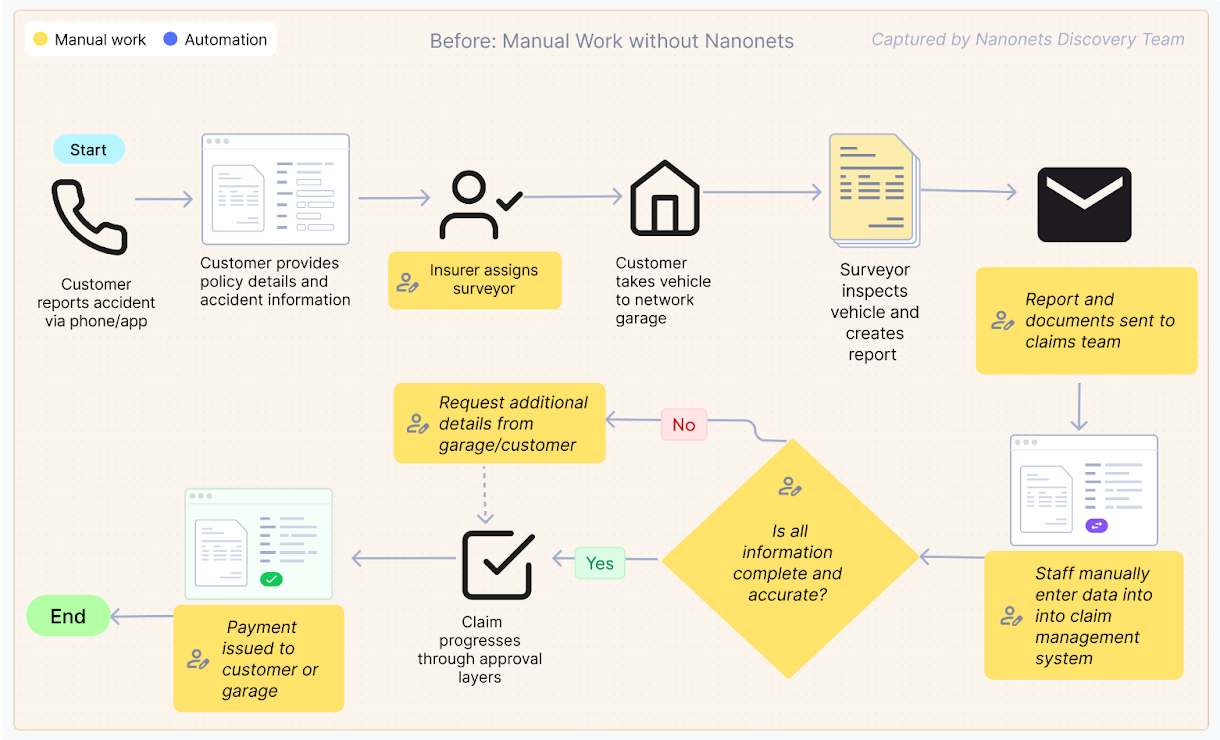
1. When an accident happens, the client can both name up the insurer’s toll-free quantity to register the declare or use their proprietary cell app to finish the declare type.
2. Throughout this, prospects shall be requested to share coverage quantity, automobile particulars (make, mannequin, registration quantity, and so forth.), accident or harm particulars, and police report (if relevant).
3. The client is then requested to take the automobile to one of many insurer’s licensed community garages for inspection and restore. They should submit the required paperwork to the surveyor assigned by the insurer.
4. The surveyor would examine the automobile and put together a report, which might then be submitted to the claims crew.
5. The claims crew would then assess the surveyor’s report and the paperwork submitted, evaluating elements like automobile identification, half numbers, unit pricing, and general declare validity.
6. After the evaluation, the crew would manually enter the related particulars into the claims administration system.
7. The declare would then undergo a number of layers of approval earlier than the settlement quantity could possibly be disbursed to the client or the storage (in case, the client opts for cashless mode)
The backend crew, consisting of 40 information entry clerks and vehicle specialists, manually inputs all the important thing particulars from the declare file into their proprietary declare administration system. This included capturing data from completely different doc sorts, reminiscent of estimates, invoices, registration certificates, driving licenses, and extra.
Do not forget that these paperwork are issued by completely different sources. As an illustration, a driver’s license issued in a single state might not observe the identical format because the one issued in one other state.
The crew would meticulously evaluation every line merchandise and half quantity to make sure accuracy earlier than the declare could possibly be additional processed and authorised. One other problem was the inconsistent naming conventions for components throughout completely different garages and producers – the identical part would have completely different names relying on who submitted the doc.
As an illustration, what seems as a entrance bumper on one estimate may be listed as a bumper cowl on one other. Equally, the part known as a boot in paperwork from UK and German producers would present up as a deck or trunk in producers from different nations. With no standardized database, these variations created fixed confusion.
Mismatches in automobile identification or half numbers, incorrect unit pricing, or lacking paperwork would trigger the declare to return to evaluation. This whole course of may take wherever from 15 to 30 days, falling in need of the brand new regulatory timelines.
When claims prolonged past IRDAI’s mandated settlement durations, the implications had been each regulatory and industrial. On the regulatory facet, the insurer confronted financial penalties and present trigger notices. Commercially, these delays broken their market fame and prompted formal buyer complaints, which require important time and assets to resolve. The prolonged processing drove up operational prices, as claims wanted further touchpoints and extended dealing with, additionally leading to buyer dissatisfaction.
The insurer rapidly realized that this inefficient workflow couldn’t sustain with the rising enterprise calls for and the stricter regulatory necessities.
How the insurer automated its declare processing workflow
The insurer knew they needed to step up their recreation. Among the opponents, particularly the absolutely digital-first insurers, had already began rolling out zero-touch declare processing.
They explored a number of OCR options, however rapidly realized such instruments received’t reduce it. These instruments had been closely depending on format and construction consistency. This led to formatting errors and inconsistent extraction, and extra guide interventions. And to make issues worse, they might solely feed sure doc codecs into the system, leaving a good portion of the declare information untouched.
The insurer found out they wanted a format-agnostic resolution that might deal with all doc sorts, extract the best data, and combine seamlessly into their present claims administration system. After evaluating a number of AI-powered doc processing platforms, they selected to go along with Nanonets’ Clever Doc Processing (IDP) resolution.
Right here’s why:
- Simplicity of the PDF extraction workflows
- Line merchandise extraction accuracy
- API and system integration capabilities
- Capacity to deal with all doc codecs, together with handwritten and semi-structured paperwork
- Multi-lingual capabilities
We at Nanonets labored with the insurer to create a tailor-made doc processing resolution that match their particular claims workflow. The implementation targeted on incremental enhancements fairly than a whole in a single day transformation.
The crew started by tackling essentially the most crucial paperwork within the claims course of: estimates, invoices, and pre-invoices. These paperwork comprise the important details about automobile damages, required repairs, and related prices.
The preliminary section targeted on:
- Configuring OCR fashions to extract line objects from restore invoices and estimates
- Creating programs to tell apart components from labor prices
- Constructing validation guidelines to flag potential information inconsistencies
- Integrating with the insurer’s utility on their proprietary declare administration system by way of API
The workflow was simple. Right here’s what it regarded like:
- Declare initiation and doc assortment: When a declare occasion happens, policyholders provoke the declare type by the insurer’s consumer interface or customer support. The declare type collects fundamental particulars together with important paperwork together with restore estimates, invoices, and supporting documentation.
- Doc submission to Nanonets: As soon as uploaded to the insurer’s system, these paperwork are mechanically routed to Nanonets by way of API integration. Beforehand, a crew of 40 backend workers would manually evaluation and enter data from these paperwork into their system.
- Clever doc processing: Nanonets processes the paperwork utilizing specialised fashions to:
- Classify every doc kind mechanically (bill, estimate, registration certificates, and so forth.) and route it to the best information extraction mannequin
- The mannequin extracts structured information from each standardized and non-standardized codecs
- Learn and manage line objects from restore estimates and invoices
- Distinguish between components and labor costs utilizing key phrase recognition
- Elements database validation: Extracted half data is validated in opposition to a complete components grasp database that:
- Standardizes various half names throughout completely different garages (bumper vs. cowl)
- Identifies potential baby half replacements (reminiscent of door pores and skin versus whole door meeting)
- Categorizes supplies (plastic, glass, steel) for correct value evaluation
- Information integration: The extracted and validated data is shipped again into the insurer’s system as a customized JSON file, mechanically populating the suitable fields within the declare evaluation interface.
- Exception-based evaluation: The backend crew evaluations the populated information, focusing solely on flagged exceptions or uncommon circumstances.
- Approval and settlement: Claims that go validation proceed to approval and settlement, with considerably decreased guide intervention.
The preliminary implementation targeted on core paperwork (estimates, invoices, and pre-invoices), with plans to develop to supporting paperwork like driving licenses, registration certificates, journey permits, health certificates, and tax paperwork.
The affect of automating insurance coverage claims processing
It’s been solely three months for the reason that implementation, however the brand new workflow has already proven promising indicators for the insurer.
Let’s check out the affect:
- 1.5 million pages processed in three months, nearly double the earlier quantity of 760,000 pages
- Standardized naming for about 600 widespread components that cowl 90% of claims
- Systematically determine alternatives for baby half replacements (like a door pores and skin at ₹5,000 versus a whole door meeting at ₹20,000) – saves a ton of value
- Allow employees to spend much less time on information entry and extra on doc evaluation and exception dealing with
- Simpler to fulfill IRDAI’s regulatory timelines, which require declare selections inside 7 days of receiving the survey report
- Customized JSON integration permits seamless information movement between Nanonets and the insurer’s declare administration system
Proper now, the main focus is on the core paperwork — estimates, invoices, and pre-invoices — because the crew will get snug with the brand new course of. After that, we’ll cowl the remaining doc sorts like driving licenses and registration certificates within the subsequent section — this could reduce guide work by 50%.
What’s subsequent
The following section will develop doc processing to incorporate supporting paperwork like driving licenses, registration certificates, journey permits, health certificates, and tax paperwork. Moreover, we’re working with the identical insurer, automating their medical claims processing workflow.
In case your insurance coverage firm is struggling to cope with mounting paperwork and lacking regulatory deadlines, we will help. Nanonets works along with your present programs to ship actual enhancements with out turning your operation the other way up. Able to see it in motion? Schedule a demo at this time.

